While it’s vitally important to bring vaccines for diseases such as tuberculosis to developing nations, getting them there is only part of the challenge. Because these countries often have unreliable infrastructures, it’s entirely possible that the vaccines can’t consistently be kept as cold as is required. As a result, they could be rendered ineffective. Now, however, scientists from King’s College London have succeeded in containing a dried live vaccine in a microneedle array, that doesn’t need to be refrigerated.
Microneedle arrays themselves have been around for a few years. They typically consist of a small patch, that has a grid of tiny sharp points on its underside. Those points are made from a non-toxic dissolvable polymer (or another biodegradable material), that has a medication mixed into it. When the patch is placed against the skin, the points painlessly penetrate its top layer, then dissolve and release the medication into the body.
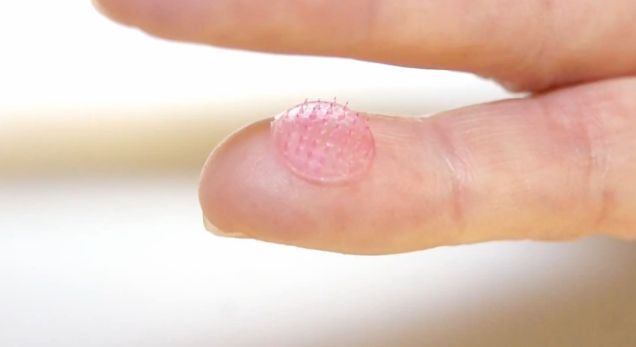
The King’s College team started with silicone microneedle array molds, into which they poured liquified sucrose mixed with a dried version of a live modified adenovirus-based candidate HIV vaccine. Once the mixture dried, they removed it from the molds, and applied the resulting patches to the skin of lab mice. The scientists observed that specialized dendritic cells in the animals’ skin triggered an immune response – which is of course the whole purpose of a vaccine.
That immune response was reportedly equivalent to one which would be induced by a liquid vaccine that had been kept at a temperature of -80ºC (-112ºF). By contrast, the microneedle arrays were kept at room temperature.
“This work opens up the exciting possibility of being able to deliver live vaccines in a global context, without the need for refrigeration,” said Dr. Linda Klavinskis. “It could potentially reduce the cost of manufacturing and transportation, improve safety (as there would be no loss in potency), and avoids the need of hypodermic needle injection, reducing the risk of transmitting blood-borne disease from contaminated needles and syringes.”

Additionally, as with all microneedle arrays, trained medical personnel wouldn’t be required to administer them, and because they’re painless, more people would likely be willing to get vaccinated.
A paper on the research was published this week in the journal Proceedings of the National Academy of Sciences. More information is available in the video below.
Source: King’s College London






