The impacts of a concussion can be felt long after the initial incident takes place, with the injury sometimes leading to severe neurodegeneration and conditions like Parkinson’s or chronic traumatic encephalopathy (CTE). In the quest to develop a treatment for these kinds of traumatic brain injuries, engineers at the University of Wisconsin-Madison (UW) have found that cooling concussed brain cells can protect them from damage and allow them to operate as normal.
“There are currently no effective medical treatments for concussions and other types of traumatic brain injuries,” says Christian Franck, an associate professor of mechanical engineering at UW-Madison who led the study. “We’re very excited about our findings because they could potentially pave the way for treatments we can offer patients.”
Franck and his team made their breakthrough by experimenting with brain cells in a dish. When brain cells are subjected to a traumatic impact, one of the consequences can be the switching on of a biochemical pathway that drives neurodegeneration and eventually the loss of cell function. The researchers set out to find ways of intervening in this process as a way of preventing the long-term damage associated with concussion injuries.
“These pathways are like flipping on a bad molecular switch in your brain,” says Franck.
To recreate these biochemical pathways in the lab, the researchers built networks of neurons in a dish. They then recreated the process of a brain injury through mechanical stimulus, which injured the cells in a similar way to a real-world concussion. The cells were then promptly cooled to a range of different temperatures and for different periods of time to find the optimal approach.
For the best results, the team found that the cooling needed to commence within four hours of the injury, and be maintained for at least six hours, though even as little as 30 minutes showed some advantages. Cooling to a temperature of 91.4 °F (33 °C) offered the most protective benefit.
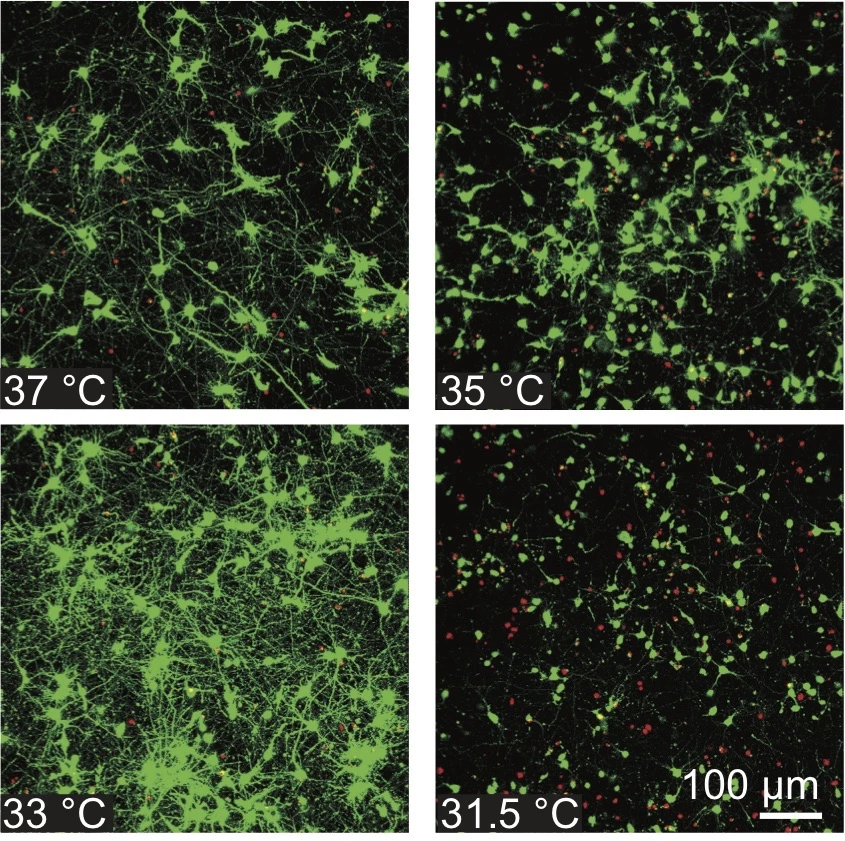
Following this method, the team found that it could keep the relevant biochemical pathways switched off and keep the cells functioning normally. Notably, they found when the brought the cells back to a normal body temperature following six hours of cooling, the pathways remained turned off.
“The biggest surprise was that the molecular switches actually stayed off – permanently – through the duration of the lab experiment,” Franck says. “That was huge.”
How this would work in a clinical setting isn’t entirely clear. The researchers note that cooling a patient’s entire body is perhaps not a viable option, as this brings risks relating to the heart and immune system. For now, the team is hoping to conduct further studies in animals to better understand the mechanisms at play.
“We hope our paper will spawn renewed motivation and interest in solving the technical challenges for getting this type of treatment to patients in the future,” Franck says. “For a long time, the scientific literature was inconclusive on whether this would be a successful treatment. What we showed in our study was that, yes, as far as the cell biology is concerned, this is effective. And so now it’s really worth thinking about how we might implement this in practice.”
The research was published in the journal PLOS One.
Source: University of Wisconsin-Madison





