Thanks to the magic of modern science, surgeons are able to remove failing livers and replace them with healthy ones from suitable donors, but they work within a pretty small window of opportunity. How long these donated livers can be safely kept on standby has a direct effect on success rates of these time-sensitive procedures, but scientists have developed a new supercooling technique that could greatly improve outcomes by taking the organs into the realm of subzero temperatures for the first time.
Storage of donated livers is something of a delicate balancing act. The cooler the temperatures the better the tissues will be preserved, but only up to a point. Freezing them or keeping them in frigid conditions for too long causes irreparable damage to the cells and makes the donated liver unusable, meaning it has to be discarded instead.
So the sweet spot for donated livers sits above freezing at 4 to 8° C (39.2 to 46.4° F), with the organs able to be held at that temperature for up to nine hours outside the human body before damage starts to occur. This strongly dictates how far the organs can travel to patients in need, how well patients can be prepared for surgery, and how well donors can be matched with recipients.
Back in 2014, scientists working at Massachusetts General Hospital came up with a way of reducing rat livers to subzero temperatures for days without causing tissue damage. By adding an antifreeze ingredient and glucose compound to the protective solution the organs are stored in, they found they could take the livers as low as -6° C (21.2° F) without freezing them, and maintain their viability for up to four days.
But scaling this supercooling technology up to take on a human liver presented some significant challenges, mostly related to how much larger the organ is. This bulkier size makes the human liver much more susceptible to the formation of ice crystals as it is cooled, which render it unusable. At the time, many saw this as an insurmountable roadblock, as Harvard Medical School research fellow, Reiner de Vries, explains to New Atlas.
“Despite our previous successes in rat livers, the likelihood of ice formation during supercooling increases with volume which made experts in the field, including us, question if this technique would ever be applicable to human livers, which are 200 times larger in size,” he says.
But Reiner de Vries and his colleagues at Massachusetts General Hospital kept tinkering with the technology and have now made a massive breakthrough. The advance involves a few tweaks to the method, starting with the complete removal of air from the organ storage bag, which eliminates the chances of ice crystal formation. They also threw a couple more additives into the mix: trehalose, which protects and stabilizes the cell membrane, and glycerol, which supercharges the glucose compound added in the 2014 study.
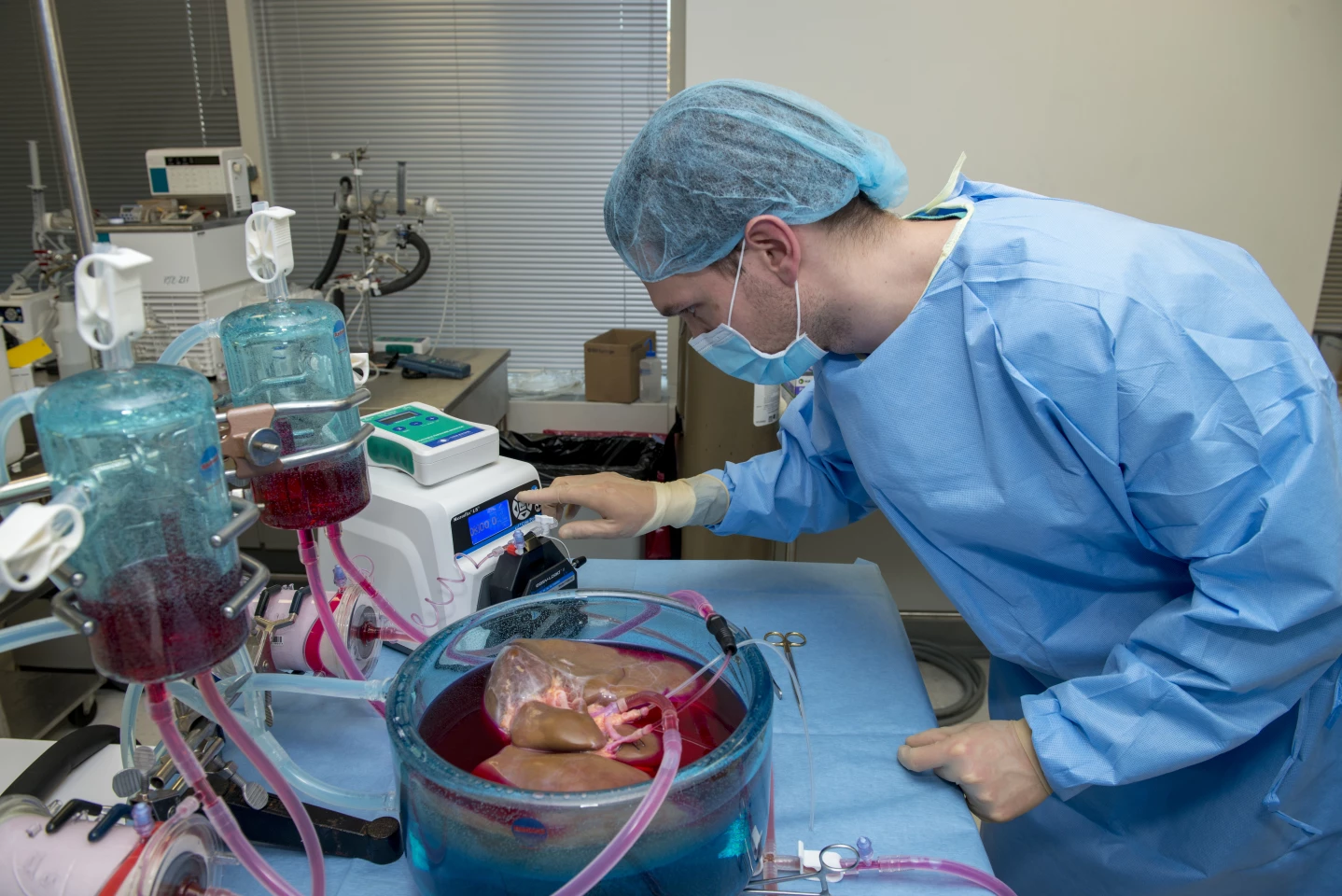
What the scientists were left with, however, was a far thicker, more viscous solution to store the organ in, which threatens to damage the cell linings inside the blood vessels and would be harder to distribute evenly throughout the organ. So to overcome these dilemmas, the team turned to a technique called machine perfusion, which is commonly used to deliver oxygen and nutrients to donor organs outside the body.
By slowly lowering the temperatures and dialing up the concentration of their cocktail of additives, the scientists were able to safely supercool the liver tissue and store it at -4° C (24.8° F). Very cool indeed. But even cooler, this extends the viability of the tissues from nine hours to 27 hours, which is nothing short of a game-changer when it comes to organ transplantation.
“Transplantation is a race against the clock,” de Vries tells us. “With the extra time we can take at least some of the stress off the transplant team and allow more time for a patient to be prepared for the transplant. Also, the transplants can be planned during the day and don’t have to be performed in the middle of the night when an organ comes available. Finally, the distances over which organs can be shared here would be much bigger. Currently we can only share organs locally. With the extra time for transport the organs can be transported throughout the US and even beyond. This will have enormous benefits for the matching of the donor and the recipient.”
While the possibilities are hugely exciting, we’re not quite there yet. The team hasn’t actually transplanted a human liver stored in this way, though say that the standard methods of assessing liver viability suggest it will be perfectly safe. The researchers are hopeful of developing a portable device that can be taken to donor hospitals to supercool the organs immediately after removal, which they expect would stretch the storage time even further.
Equally exciting is the possibilities this breakthrough could mean for organ transplants as a whole. As of January this year, there were more than 113,000 patients on the national organ transplant waiting list in the US, with 20 dying each day. As it turns out, in the human liver the scientists may have chosen the ideal testbed to develop their organ cooling technology, though there is still work to be done.
“It's a breakthrough that we can now successfully supercool human livers,” says de Vries. “Moreover, the liver is the largest solid organ in the human body and therefore it is very likely that it also can successfully prevent ice during storage of much smaller organs such as kidneys hears, ovaries etc. But this has yet to be tested.”
The research was published in the journal Nature Biotechnology.
Sources: Harvard Medical School, National Institute of Health







