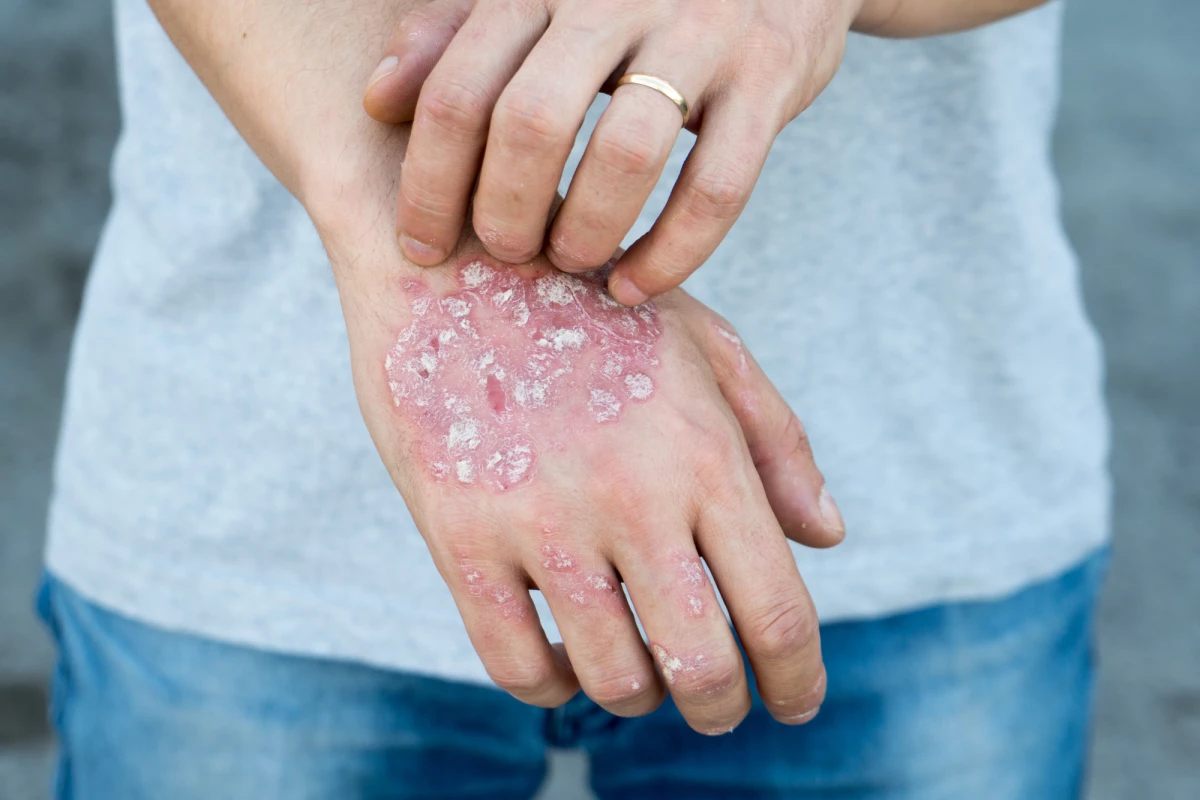
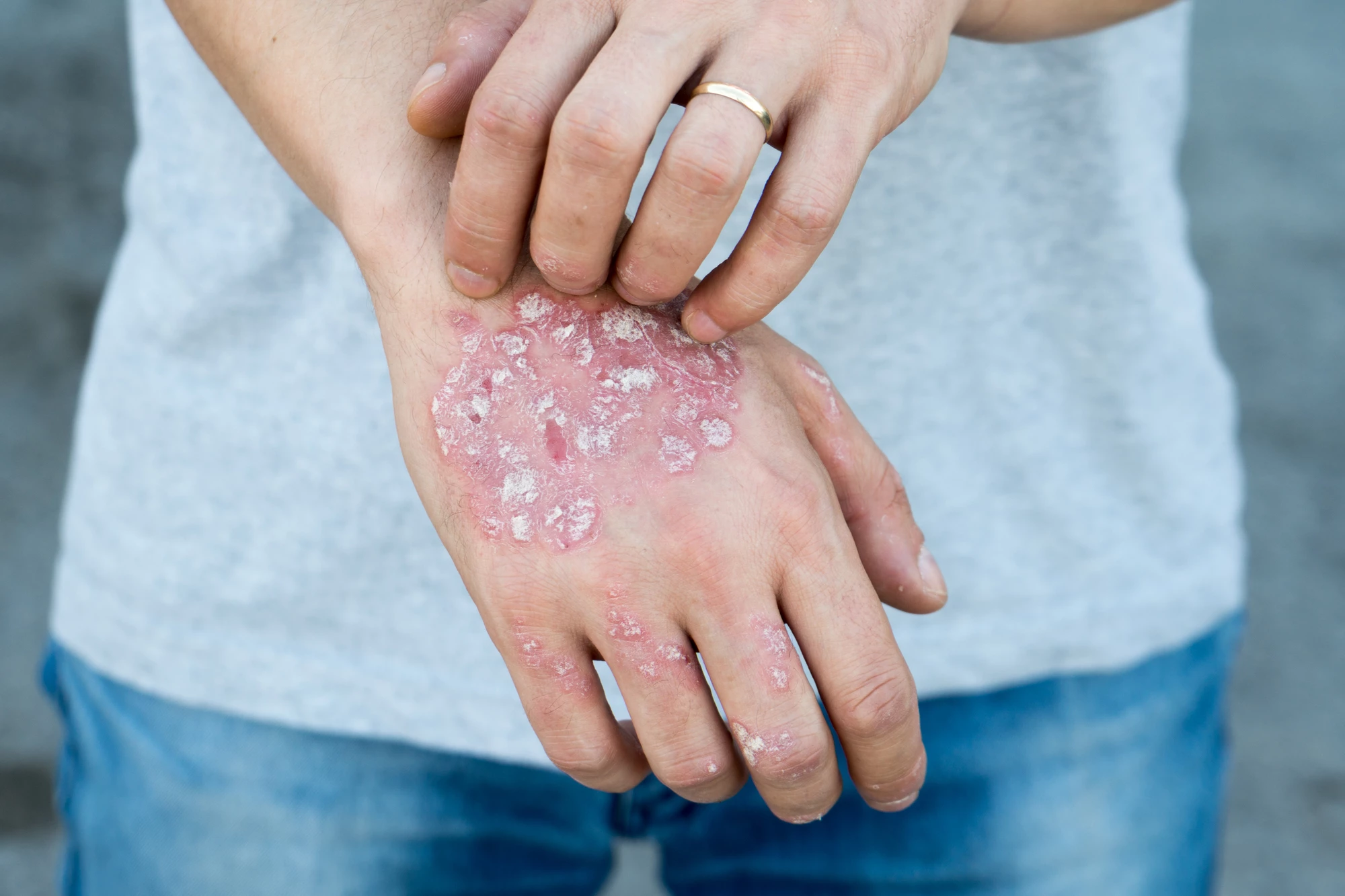
Researchers have identified a way of selectively eliminating the ‘bad’ immune cells that contribute to autoimmune skin diseases, while leaving the ‘good’ cells intact. The discovery could lead to longer-lasting, more targeted treatments for conditions like psoriasis and vitiligo.
Our skin contains specialized immune cells that protect us against infections and cancer and promote healing. These long-lived tissue-resident memory (TRM) T cells are so-called because, unlike other immune cells, they stay put in the skin tissue and don’t circulate in the blood. But, if they’re not properly controlled, TRM cells can contribute to autoimmune skin diseases like psoriasis and vitiligo.
Now, a study led by researchers at the University of Melbourne and the Doherty Institute of Infection and Immunity (Doherty Institute) has uncovered the unique elements that control various types of skin TRM cells in animal models, providing them with a means of selectively eliminating the problematic cells.
“Specialized immune cells in our skin are diverse: many are critical to prevent infection and cancer, but others play a big role in mediating autoimmunity,” said Simone Park, lead and co-corresponding author of the study. “We discovered key differences in how distinct skin T cells are regulated, allowing us to precisely edit the skin’s immune landscape in a targeted way.”
There are two important TRM cell subsets found in human skin: interferon-gamma-producing CD8+ (TRM1) cells, which have antiviral and anticancer roles, and interleukin-17-secreting CD8+ (TRM17) cells. While both can contribute to skin pathologies, the researchers found that, in mice, TRM1 and TRM17 cells navigate different signaling pathways that set them on a trajectory to acquire residency in the skin tissue. Furthermore, they found that TRM17 cells could be selectively eliminated by targeting elements of their signaling pathway without compromising their TRM1 counterparts.
“Most autoimmune therapies treat the symptoms of the disease rather than addressing the cause,” said Susan Christo, one of the study’s co-authors. “Conventional treatments for skin disorders often impact all immune cells indiscriminately, meaning that we could also be wiping out our protective T cells. Until now, we didn’t know how to pick apart ‘bad’ T cells in the skin from the ‘good’ protective ones. Through this research, we discovered new molecules that allow us to selectively remove disease-causing T cells in the skin.”
The researchers say their findings could lead to more precise, long-lasting therapies for skin disease.
“Skin conditions like psoriasis and vitiligo are difficult to treat long term,” said Laura Mackay, a co-corresponding author. “The T cells driving disease are hard to remove, so patients often need life-long treatment. Our approach has the potential to revolutionize the way we treat these skin disorders, significantly improving outcomes for people dealing with challenging skin conditions.”
Further research is needed on human subjects to validate the efficacy of these strategies.
“These discoveries bring us one step closer to developing new drugs that durably prevent autoimmune skin disorders without compromising immune protection,” Park said.
The study was published in the journal Science.
Source: Doherty Institute