Although conditions such as epilepsy and chronic pain can be treated via nerve-stimulating implanted electrodes, those electrodes are stiff, expensive and require surgery to implant. Scientists have now created an alternative, however, in the form of soft, injectable electrodes.
The so-called "injectrode" technology is being developed by biomedical engineers at the University of Wisconsin-Madison. At the heart of their system is a liquid silicone that's similar to surgical glue, and which contains metal nanoparticles to make it electrically conductive.
After being injected around a target nerve, that silicone cures within the body, taking on a flexible, stretchable consistency not unlike that of biological tissue. As a result, unlike a rigid electrode, the material is able to twist and stretch with the body, instead of breaking or coming loose.
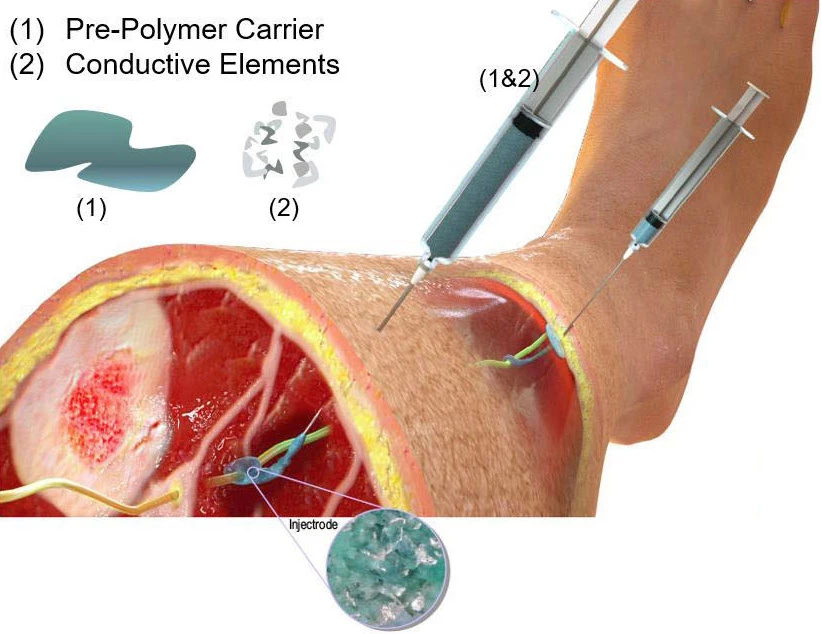
And while the bulk of the injectrode sits around a nerve deep within the body, some more of the silicone is deposited just beneath the skin, with a thin insulated trail of the material connecting the two areas. Utilizing a regular store-bought transcutaneous electrical nerve stimulation (TENS) unit, it's subsequently possible to electrically stimulate the nerve through the skin whenever needed.
By contrast, applying an electrical current to traditional rigid electrodes is a considerably more costly and complex process, typically involving an implanted power source.
So far, the scientists have utilized their system to induce heart rate changes in pigs by stimulating their vagus nerve – stimulation of that nerve has previously been put forward as a means of treating conditions such as heart failure and hypertension. The technology has also been subjected to a number of Food and Drug Administration preclinical tests, with an eye toward eventual human trials.
"As we learn more and more about how to interface with the nervous system, we're not limited to what we've implanted through an invasive surgical procedure," says Assoc. Prof. Kip Ludwig, co-author of a paper on the study. "We can actually change how we stimulate, how we talk to the nerve, because we're essentially just routing our connection to this deep nerve back to the surface of the skin."
The paper was recently published in the journal Advanced Healthcare Materials. Ludwig and colleagues are now commercializing the injectrode system, through their biotech startup Neuronoff.
Source: University of Wisconsin-Madison




