When someone overdoses on opioid drugs, which is happening increasingly often, an injection of naloxone could save their life … if it's administered soon enough. A wearable system that's currently in development is intended to make that happen automatically.
Although drug-users can give themselves naloxone injections after overdosing, the problem is that they're often so incapacitated that they're unable or unwilling to do so. The opioid thus proceeds to bind with their brain receptors that regulate breathing, causing them to hypoventilate (breath inadequately), which in turn results in death.
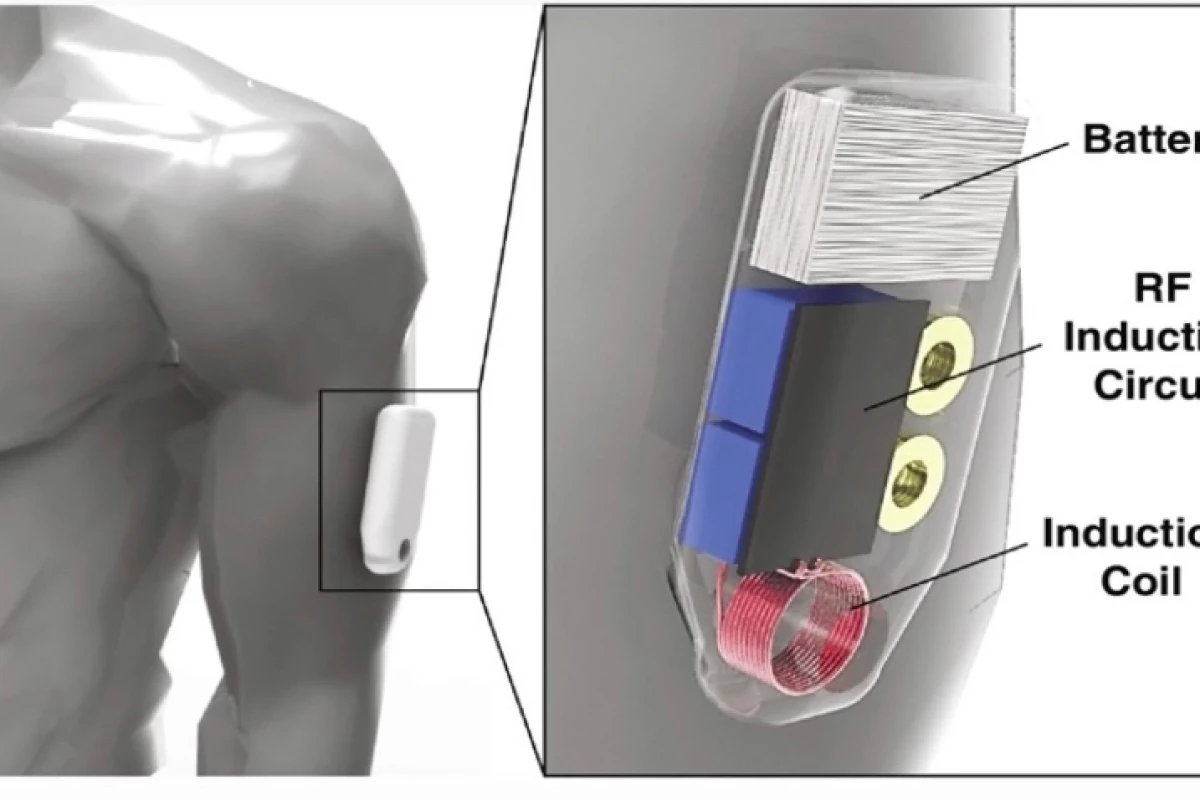
Led by Asst. Prof. Hyowon "Hugh" Lee, scientists at Indiana's Purdue University decided to do something about this problem, designing an automated naloxone-delivery system that's on/in the at-risk person at all times. It consists of three main parts: a battery-powered magnetic armband, an adhesive EKG sensor, and a naloxone capsule that's injected under the arm skin ahead of time, in an outpatient setting.

When the wearer overdoses and begins hypoventilating, the EKG sensor will detect that their rate of respiration has fallen dangerously low. It will respond by sending a signal to the armband, which will in turn respond by using its induction coil to create an alternating magnetic field.
Extending below the skin beneath the armband, that field will cause a strip of stainless steel in the capsule to heat up. That heat will cause the capsule to melt, releasing the naloxone into the bloodstream. The whole process should take place within 10 seconds.
Ultimately, the system may also automatically contact emergency services – although naloxone buys drug users about an hour in the event of an overdose, they still need to receive proper treatment at a hospital.
The researchers are now working on making the system less bulky, plus they're looking at adapting it to deliver other types of medication in response to other problems. It could, for instance, administer epinephrine when a dangerous allergic reaction occurs.
A paper on the research was recently published in the Journal of Controlled Release.
Source: Purdue University