Injured cartilage can take the body a long time to repair, but back in 2014 we looked at a promising study where scientists created grafts from nasal cartilage cells and deployed them in damaged knees to help things along. The researchers have since taken some exciting strides forward with their technology, most recently demonstrating how the engineered nasal tissue can not only act as structural reinforcement for troublesome joints, but also how its unique properties can counter inflammation in severe osteoarthritis.
The research is the work of scientists at Switzerland's University of Basel, and looks to harness some of the unique capabilities of cells found in the nasal septum, the cartilage in between the nostrils. One thing that separates these cells from those found in articular cartilage in the joints is that that they lack certain genes that inhibit reproduction, meaning they can grow and form cartilage far more easily. Conveniently, this remains the case even as we age, meaning that they could theoretically be used as treatments for deteriorating joints in elderly people.
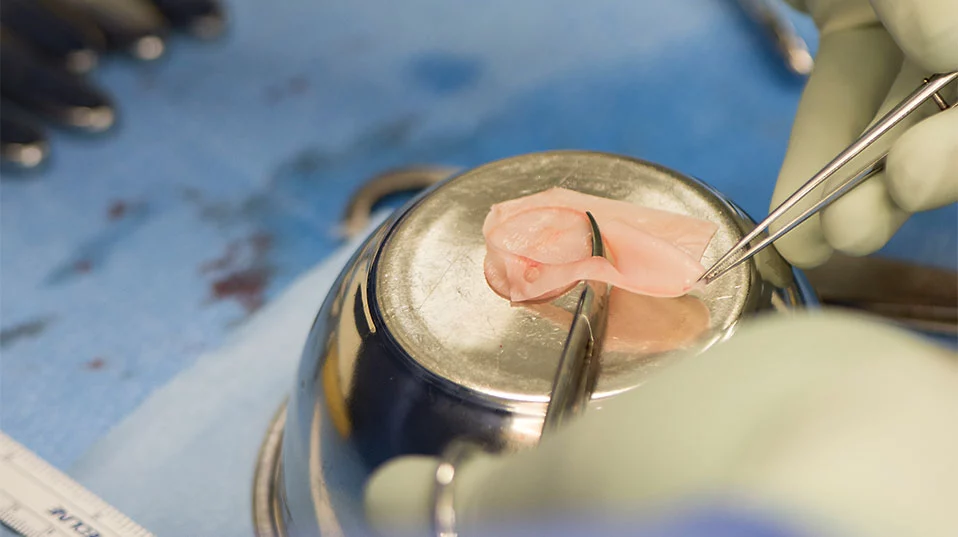
In their 2014 study, the scientists led by Professor Ivan Martin harvested pieces of cartilage from the nasal septum of test subjects, extracted cells from that tissue and then applied them to a biocompatible scaffold. In colonizing the scaffold, the growing cells formed a graft, which was then successfully used to replace damaged articular cartilage in a subject's knee, where it proved capable of enduring the high mechanical load. But using the technology to take on the degenerative joints caused by osteoarthritis presents another challenge entirely.
"The situation in osteoarthritis is even more challenging since it is characterized by persistent inflammatory reactions," Martin explains to New Atlas. "We had to investigate if the engineered tissue could resist and not be attacked and degenerated by the inflammatory factors."
This chronic inflammatory tissue sets osteoarthritis apart from some other cartilage defects or injuries, so there was some uncertainty around how the grafts would perform in this hostile environment. The scientist started out by subjecting their engineered cartilage to inflammatory factors in laboratory models of osteoarthritis and in animals. This included testing its ability to endure both the mechanical stress and inflammation by deploying it in osteoarthritic knee joints of sheep, and the results were encouraging.
The scientists found that not only did the engineered cartilage stand up well under these conditions, it actively neutralized some of the inflammatory reactions at play. Digging into the reasons why, the scientists came across a plausible explanation for this effect, relating to the unique plasticity and regenerative abilities of nasal cartilage cells.
"This effect could be due to the fact that a molecular signaling pathway, the WNT signaling pathway, was repressed by the presence of the nasal cartilage cells," Martin says. "This pathway is chronically upregulated in osteoarthritis and attributes to the higher expression of inflammatory factors. Repressing this pathway could possibly account for the ability of nasal chondrocytes to counter the inflammatory conditions."
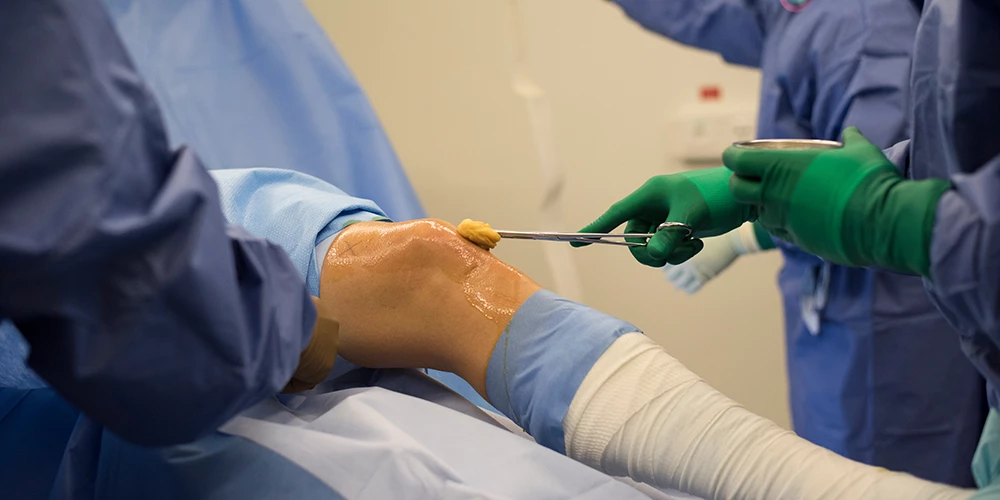
Following their successful experiments on animals, the scientists then tested out the technique on two young patients with severe osteoarthritis, who received implants of cartilage engineered from their own nasal cells. Both subjects reported a decrease in pain and an improvement in quality of life, with MRI scans of one showing that the bones in the knee join had shifted further apart, a sign of joint recovery.
"Indeed, we discovered that tissue engineered from nasal cartilage cells proved to be robust at inflammatory conditions and even seemed to counteract the inflammatory reactions," says Martin.
From here, the scientists are looking to carry out large, in-depth clinical trials to test the efficacy of the technology in tackling various forms of osteoarthritis impacting other parts of the knee, including patellofemoral osteoarthritis, known as "runner's knee." Martin tells us they also plan to expand the treatment to tackle other joints, and have received permission to test it out in shoulders and ankles.
He and the team will also conduct further research into the precise mechanisms behind these promising functions of engineered nasal cartilage, to understand its ideal properties and which patients are best suited for treatment.
The team's latest research was published in the journal Science Translational Medicine.
Source: University of Basel




