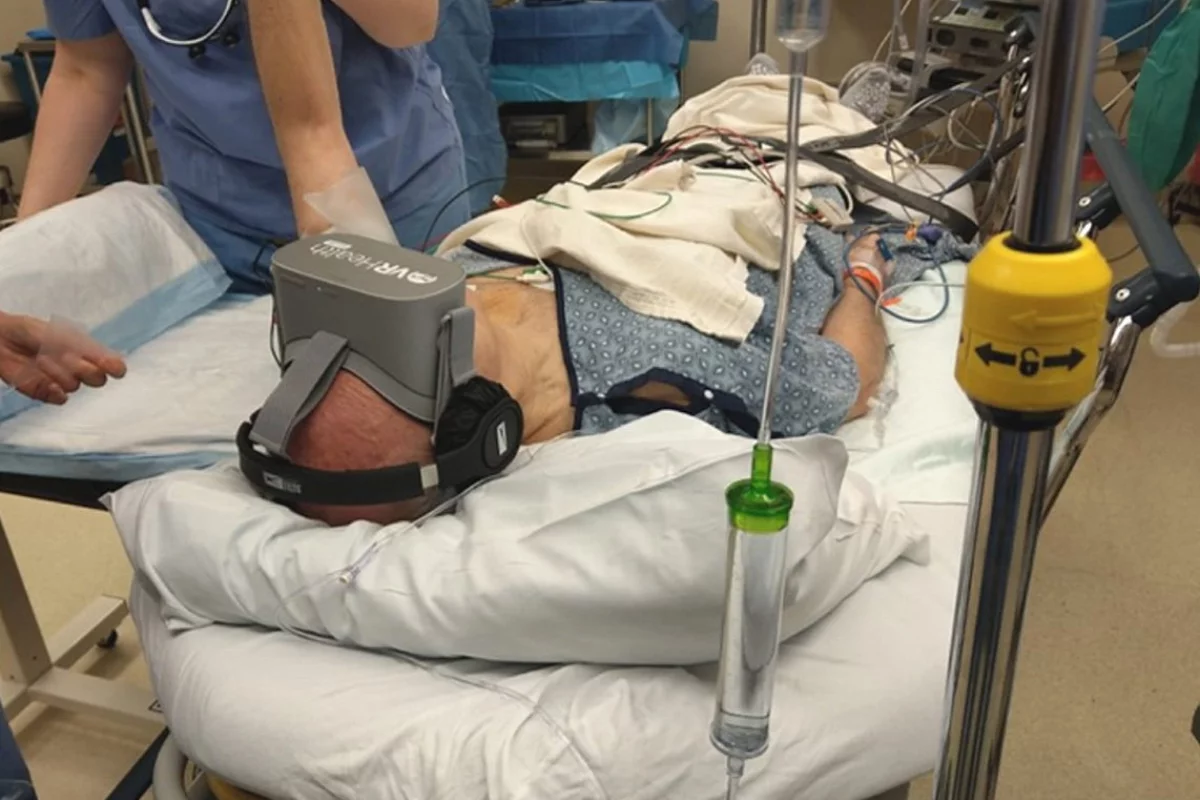
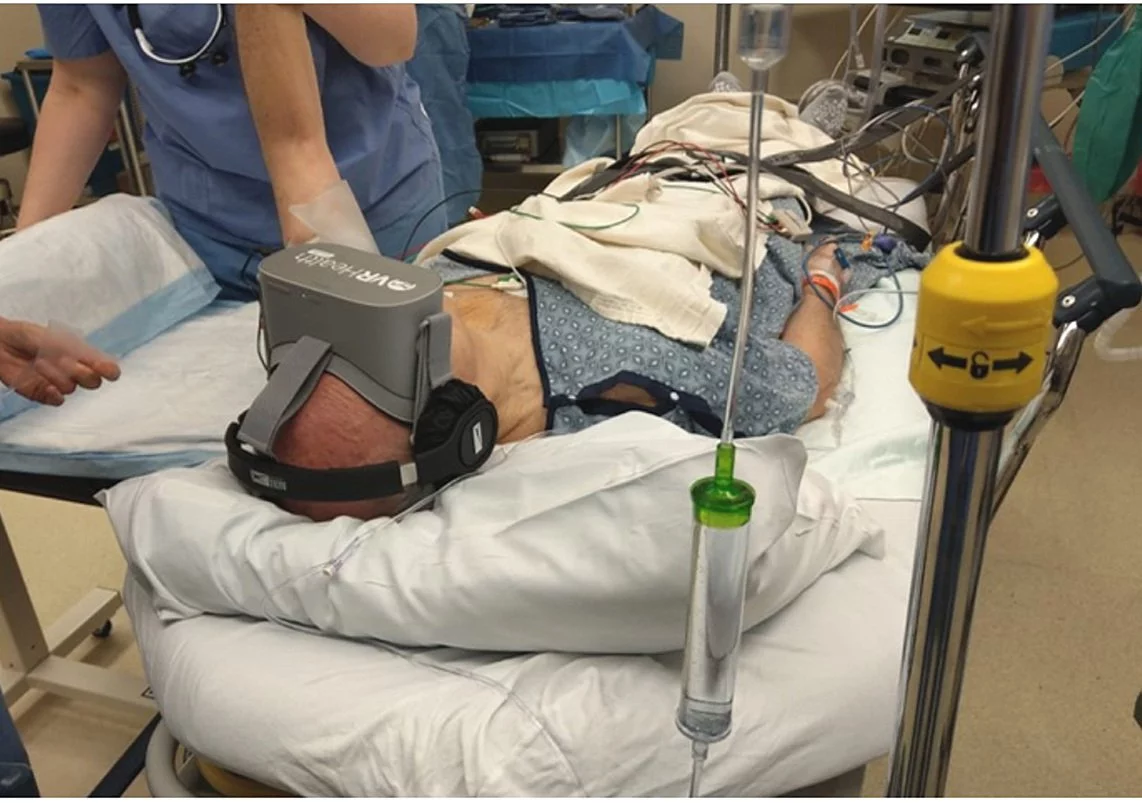
A fascinating clinical trial has reported virtual reality immersion can reduce the amount of anesthetic needed during certain types of hand surgery. The trial found patients using VR could get through an entire surgical procedure with only local anesthetic.
Researchers are exploring a number of novel medical uses for VR technology, from using VR as a tool for managing chronic back pain to incorporating it into cutting-edge psychedelic therapies. But can VR be used to replace anesthesia in surgical procedures?
As a replacement for sedation during minor procedures such as endoscopy or complex wound dressing changes VR has proved somewhat effective. However, during more serious procedures, such as orthopedic surgery, the technology has not been as successful.
In this study the researchers focused on hand surgeries, increasingly common procedures that frequently require complete unconscious sedation with a drug called propofol. Brian P. O'Gara, senior author on the new study, said modifying the amount of sedation used in these procedures will make them safer for patients and quicker to complete.
"With the increase in the amount of time people spend at the keyboard combined with our aging population, there is a projected increased need for common elective hand surgeries," said O'Gara. "Optimizing care for these patients will undoubtedly involve modification to anesthetic practices.”
The research recruited 34 patients scheduled for hand surgery and randomized them into either a VR or control group. The VR group wore a headset for the procedure and engaged in a calming experience of their choice, such as a 360-degree mountaintop environment.
The procedure started using only localized nerve-blocking anesthesia. At all stages of the surgery the patients could ask for either more local anesthetic or propofol to put them to sleep.
Only four out of the 17 patients in the VR group ultimately received propofol during the procedure, while every patient in the control group needed the more complete anesthesia. Interestingly, the VR patients ultimately used more local anesthetic in their procedures but were discharged from post-surgical care an average of 22 minutes earlier than patients in the control.
This suggests VR could offer a number of benefits to both patients and hospitals in certain contexts. Propofol sedation is not without minor risks, and in some frail patients it can lead to lingering complications.
Lighter sedation also means shorter waiting periods for patients following surgical procedures, offering hospitals more efficient protocols for dealing with higher volumes of procedures.
"Our trial is novel in that it is the first to report a significant reduction in sedative dosing with VR immersion during hand surgery on adults," added O'Gara. "Using VR immersion, the potential harms of unnecessary sedation can be avoided without compromising patient comfort during hand surgery.”
The new research was published in PLOS One.