Taking advantage of a unique public health policy in the UK, a new study has found that receiving the shingles vaccine reduces dementia risk by 20%. The findings bolster a growing body of research linking the vaccine to lower numbers of dementia cases.
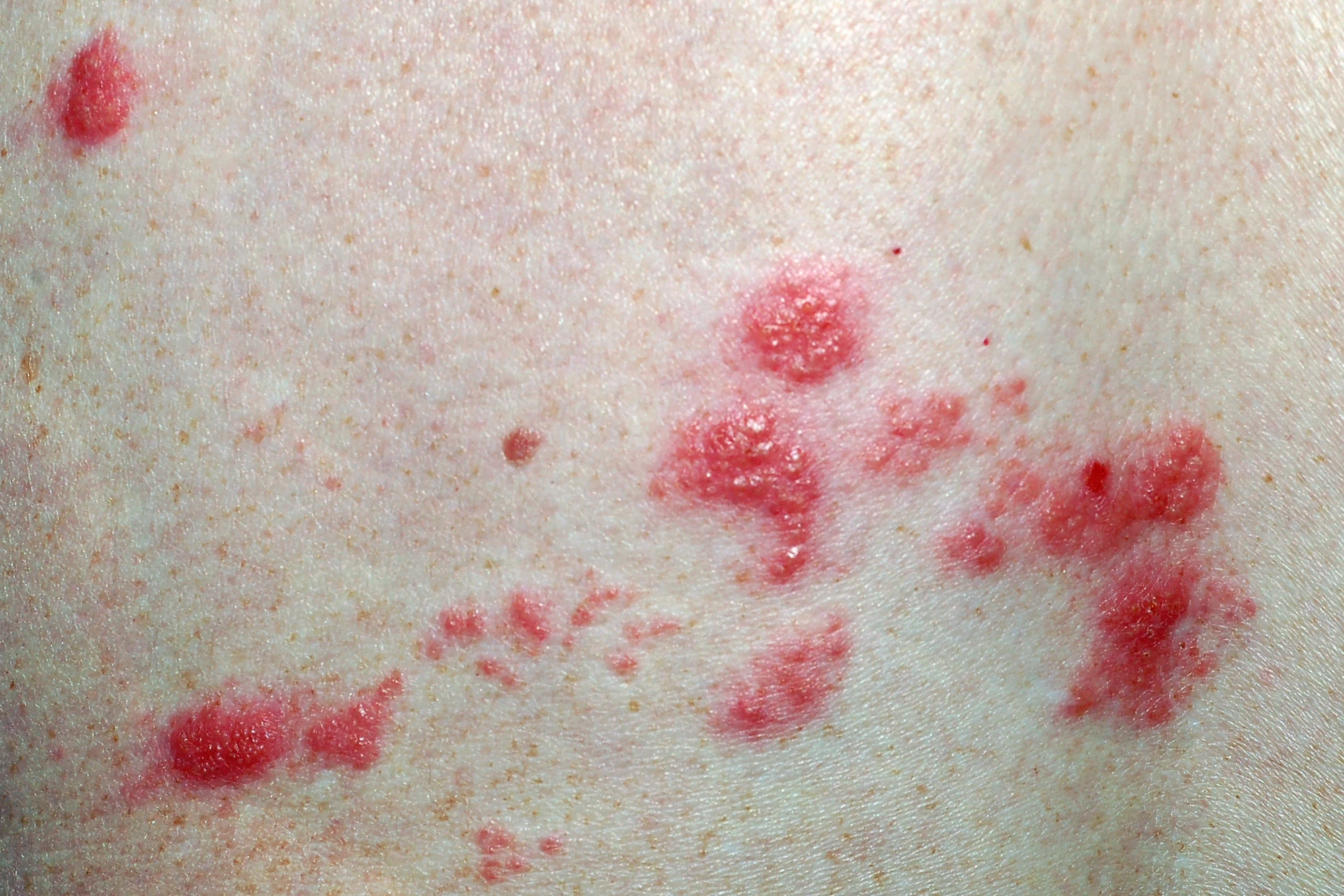
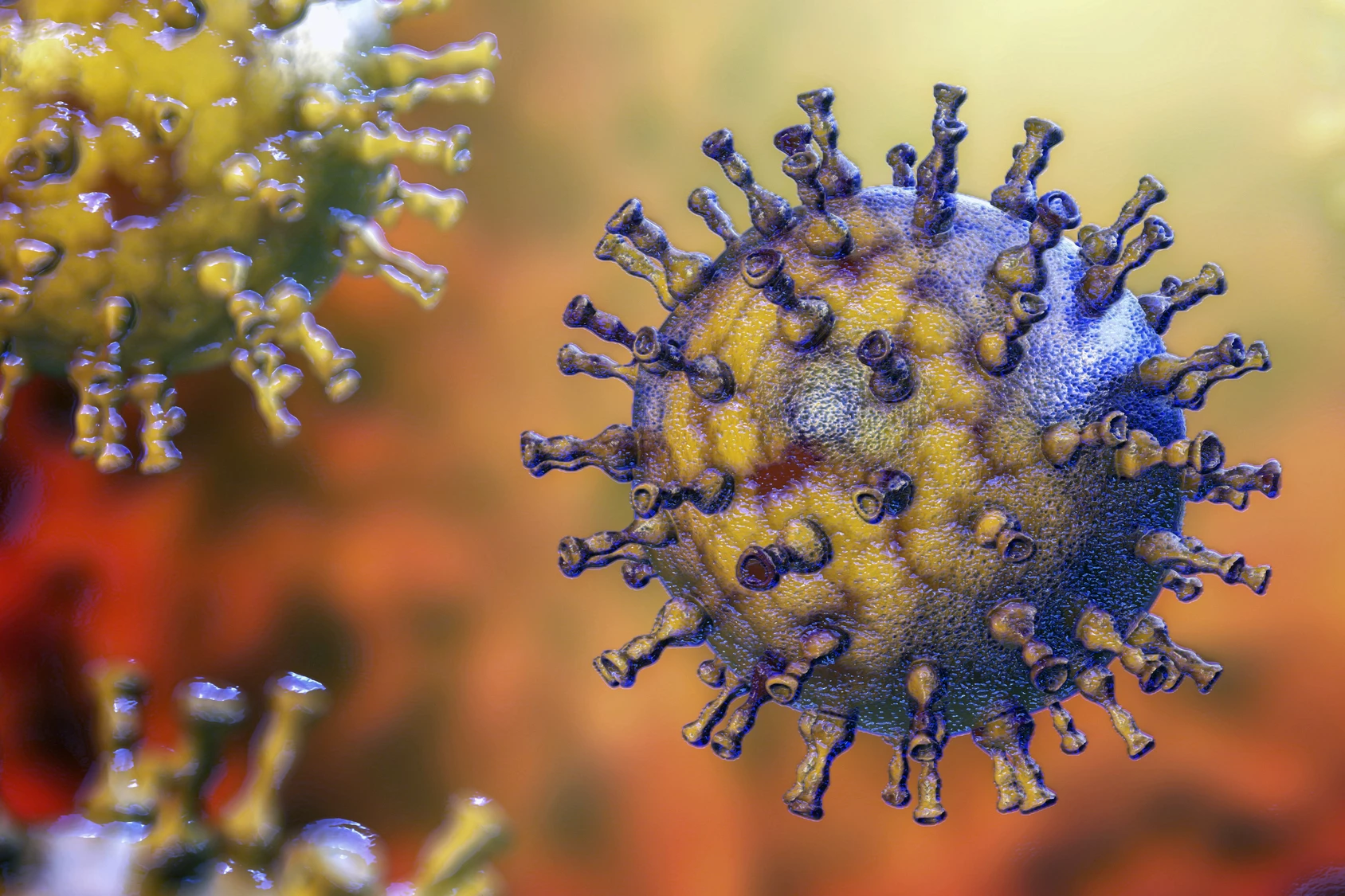
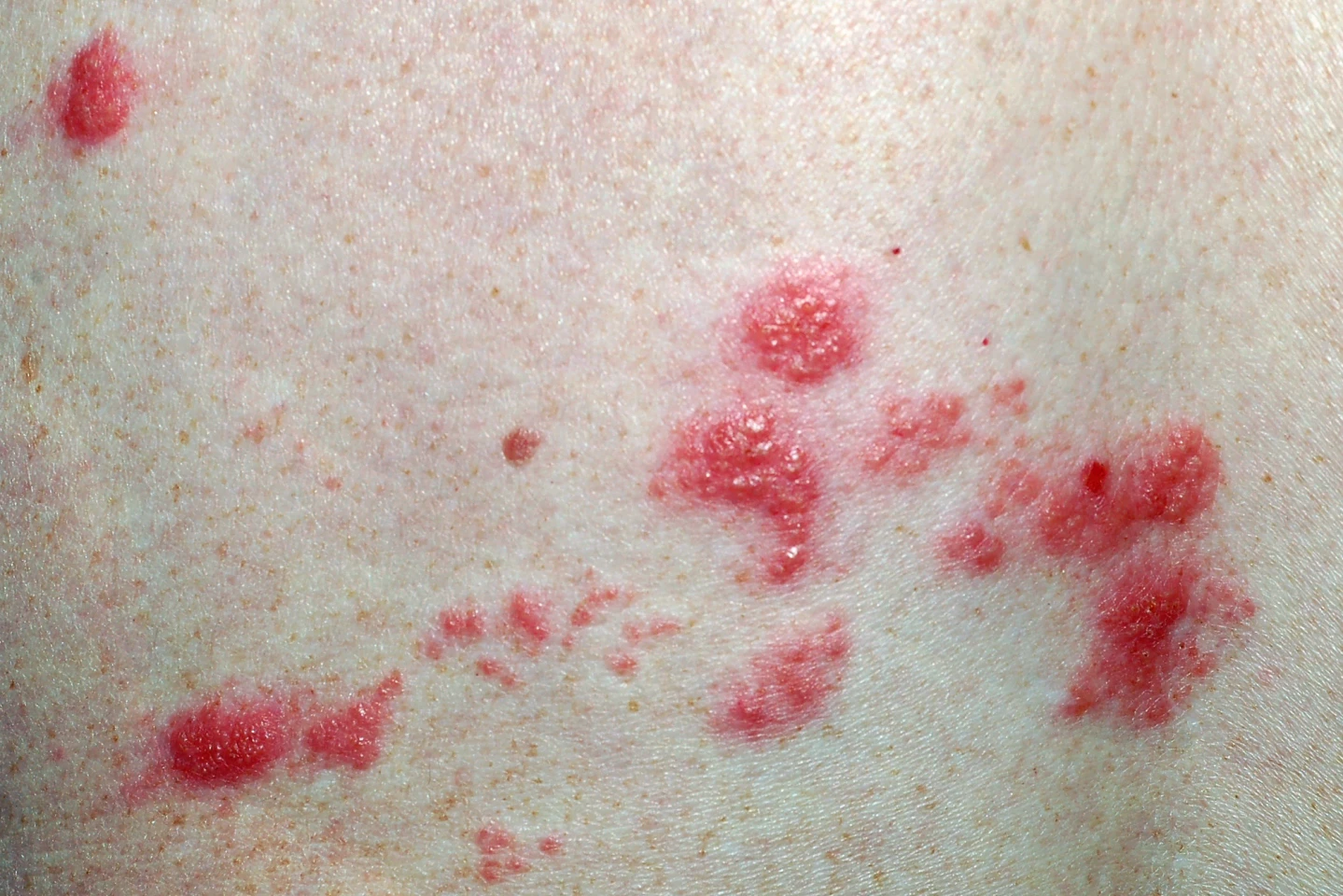
Shingles (herpes zoster) is caused by the reactivation of the varicella-zoster virus that causes chickenpox, which lays dormant in nerve cells for life, leading to a very painful, blistering rash. The risk of shingles is higher in elderly folks, where it can be more severe, with a greater likelihood of complications like persistent nerve pain and painful eye infections. For these reasons, the shingles vaccine is commonly recommended for adults aged 50 and older.
Now, a new study led by Stanford Medicine has added powerful evidence to the findings of previous studies showing a link between the shingles vaccine and lower dementia risk. But it’s done so in a unique way, thanks to the way public health policy was rolled out in Wales in the UK.
“It was a really striking finding,” said Pasal Geldsetzer, MD, PhD, assistant professor of medicine at Stanford University and the study’s corresponding author. “This huge protective signal was there, any which way you looked at the data.”
Evidence is building that herpesviruses, of which shingles is one, play a role in the development of Alzheimer’s disease. But, to date, studies investigating a link between shingles vaccination and dementia risk have only compared the occurrence of dementia in those who’d received a vaccine compared to those who hadn’t. Yes, these studies have linked getting the shingles vaccine with lower dementia rates. However, they’ve come with a major confounding bias: people who get vaccinated also tend to be more health-conscious in ways that are difficult to measure. Factors that are known to affect dementia risk, like diet and exercise, for example, aren’t included in health records.
“All these associational studies suffer from the basic problem that people who get vaccinated have different health behaviors than those who don’t,” Geldsetzer said. “In general, they’re seen as not being solid enough evidence to make any recommendations on.”
Enter Wales, the country that started rolling out its shingles vaccine program on September 1, 2013. It specified that anyone aged 79 on that date – that is, those born on or after September 2, 1933 – was eligible to receive the vaccine for at least one year. Alas, people born before that date would never become eligible. By setting these eligibility criteria, Wales had inadvertently created a unique quasi-natural experiment. Here’s why: researchers could compare individuals born immediately before the date-of-eligibility cutoff date with those eligible ones born immediately after it. Importantly, the two groups, only a few weeks apart in age, were not expected to differ significantly from one another, which would reduce the probability of confounding variables.
“We know that if you take a thousand people at random born in one week and a thousand people at random born a week later, there should not be anything different about them on average,” said Geldsetzer. “They are similar to each other apart from this tiny difference in age. What makes the study so powerful is that it’s essentially like a randomized trial with a control group – those a little bit too old to be eligible for the vaccine – and an intervention group – those just young enough to be eligible.”
The researchers obtained detailed electronic health record data from 282,541 adults who resided in Wales and did not have a diagnosis of dementia when the country’s shingles vaccine program started. Participants were followed up for seven years, with researchers comparing the health outcomes of those closest in age who were eligible to receive the vaccine. Factoring in actual vaccination rates enabled them to determine the effects of receiving the vaccination.
By 2020, one in eight participants – by then aged 86 and 87 – had been diagnosed with dementia. However, the researchers found that receiving the shingles vaccine reduced the probability of a new dementia diagnosis by 20%.
Scouring the data for other variables that might’ve affected dementia risk, the researchers found that both groups, vaccine-eligible and vaccine-ineligible, were practically indistinguishable. There was no difference in education levels. Vaccine-eligible individuals were not more likely to get other vaccines or preventive treatments, nor were they less likely to be diagnosed with other common health conditions, such as diabetes, heart disease, and cancer. A drop in dementia diagnoses was the only difference between them.
“Because of the unique way the vaccine was rolled out, bias in the analysis is much less likely than would usually be the case,” Geldsetzer said.
Determined to explore all avenues when it came to variables, the researchers used alternative methods to rigorously analyze their data, using different age ranges or looking only at deaths attributed to dementia, for example. The link between vaccination and lower dementia rates remained. They also noted a significant difference in the effect of the vaccine on dementia between the sexes, with women benefitting more than men. The researchers are not certain why this was but suggest that one reason might be that women tend to produce a stronger response to vaccines than men.
The study’s findings have drawn comments from experts who were not involved in the research.
“There has been evidence for some time that older people who receive their vaccinations, in general, are less likely to develop dementia,” said Dr Henry Brodaty, Scientia Professor of aging and mental health and co-director of the Center for Healthy Brain Aging (CHeBA) at the University of New South Wales. “This is the best evidence yet to show this. Future research will determine whether the newer non-live virus, Shingrix, will provide the same benefit and whether immunization at younger ages may be just as effective.”
That last point is an important one. The old-school vaccine, Zostavax, which is now obsolete and has been unavailable in developed countries since 2020, used a weakened live form of the virus that causes shingles, given in one dose. It mimicked a real shingles infection to teach the body’s immune system how to fight it. It was less effective than the newer vaccine, and its protection against shingles waned over time. Zostavax couldn’t be given to immunocompromised people because it contained a live virus.
The new-school Shingrix vaccine doesn’t contain a live virus. Instead, it uses a piece of the shingles virus (a protein) plus a booster ingredient called an adjuvant to spark a strong immune response. It teaches the body to recognize and respond to the virus without risking an actual infection. It’s far more effective than Zostavax, even in older adults, provides longer-lasting protection, and can be used in adults with a weakened immune system. It is given in two doses, spaced two to six months apart.
Aside from using a live-virus vaccine, experts have pointed out other limitations of the study.
“This study had an observational design, so we need to be cautious in assuming the vaccine itself caused this decline in dementia diagnosis,” said Dr Joseph Doyle, professor of infectious diseases at Monash University and President of the Australasian Society for Infectious Diseases (ASID). “It is plausible that episodes of infection, immune system changes, or health care engagement are among the factors behind this association, but further research is needed to help determine whether there is a causal link.”
But, overall, the response to the study has been positive.
“This is a landmark finding in brain health and disease prevention,” said Professor Tissa Wijeratne, a neurologist and co-founder of World Brain Day at the World Federation of Neurology. “It supports the emerging understanding that infections – especially neurotropic viruses like varicella-zoster – can contribute to long-term neurological decline …. These findings reinforce one of the most critical messages from our World Brain Day campaigns: prevention matters most.”
What isn’t clear from the present study is how the shingles vaccine exerts its apparent protective effect. That’s a matter for future research. Nonetheless, the findings of the study, which have been replicated in other countries that had similar shingles vaccine rollouts, such as England, Australia, New Zealand, and Canada, appear promising.
“Our substantial effect sizes, combined with the relatively low cost of the zoster vaccine, imply that, if these findings are truly causal, the zoster vaccine will be both far more effective as well as cost-effective in preventing or delaying dementia than existing pharmaceutical interventions,” the researchers said.
The study was published in the journal Nature.
Source: Stanford University