For sufferers of diabetes, keeping blood glucose levels within a healthy range can be a difficult and labor-intensive balancing act that often requires regular insulin injections, but some scientists imagine a future where medicine does the heavy lifting for them. A team at Indiana University School of Medicine has taken a promising step towards this future, demonstrating a type of "synthetic hinge" that swings into action when blood glucose levels call for corrective action.
The hormone insulin plays a vital role in keeping glucose at healthy levels in the blood, pulling it out of the bloodstream and helping turn it into energy. In diabetes patients, insufficient amounts or insulin that results in a reduction in effectiveness means that blood glucose levels are left to rise to potentially dangerous levels, which can have serious consequences.
Injections of insulin are a way for Type 1 diabetics to manage the condition, but one dangerous side effect of this is the potential for them to drive blood-sugar levels too low, a condition known as hypoglycemia. These concerns have moved scientists to explore a concept known as "glucose-responsive insulin," an engineered form of the hormone that would self-adjust depending on the blood sugar levels of the patient.
“The reason a glucose-responsive insulin is important is that the biggest barrier to the effective use of insulin, especially in Type 1 diabetes, is the fear of the consequences of blood sugar going too low,” says study author Michael A. Weiss.
Last year, we looked at an interesting early example of what this technology could look like. Scientists in Denmark developed a novel insulin molecule that could spontaneously increase or decrease its activity in response to circulating blood sugar levels, as demonstrated in rats. Weiss has now led the development of a technology with similar potential, albeit via a different mechanism, and one described as relatively simple.
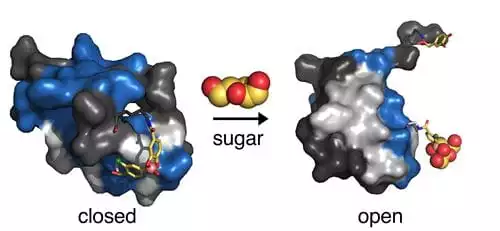
The approach leverages a naturally occurring type of "protective hinge" in insulin, which keeps the hormone stable when closed and makes it functional when open. The researchers chemically altered the molecule by adding a sugar sensor and what they call an artificial switch, which disrupts the hinge's naturally closed state and enables it to respond to fructose by opening up.
These capabilities of the "synthetic hinge" were demonstrated in lab experiments involving human-liver-derived cells, which the researchers say resulted in the appropriate hormonal signaling. In its current form, the modified insulin senses fructose and would need to be adapted to sense glucose for the purposes of diabetes treatment, and do so at levels sensitive enough to respond to fluctuating levels in the blood, but the scientists believe the potential is there.
“The promise of this kind of ‘smart’ insulin is that it would transform diabetes care, so people wouldn’t have to worry anymore,” says Weiss. “With our invention, we envision that when the blood sugar goes low, the hinge would close. But there will be much work to do to translate our proof of principle to an FDA-approved product.”
The research was published in the journal Proceedings of the National Academy of Sciences.




