A new report from the US Centers for Disease Control and Prevention (CDC) has found more than three-quarters of people presenting at a hospital with COVID-19 were either obese or overweight. The findings build on a convincing body of research suggesting disease severity is associated with an increasing Body Mass Index (BMI).
From early on in the pandemic epidemiologists noted a distinct correlation between body weight and COVID-19 severity. It perhaps was unsurprising that obesity could be linked to greater rates of hospitalization and death. After all, obesity is a common metabolic disease often linked to heart disease and diabetes; other conditions that certainly increase one’s risk for suffering severe COVID-19.
However, a series of recently published studies is illustrating just how serious a risk factor for severe COVID-19 having a high BMI actually is. In fact, other than age, being overweight may be the most dangerous factor that leads to hospitalization and death from COVID-19.
The new CDC study looked at 148,494 adults presenting at a hospital with COVID-19 in the US between March and December last year. A striking 79.1 percent of those patients were either overweight or obese.
The study interestingly found those with a BMI between 23 and 25 (near the upper end of the healthy range) were at the lowest risk of hospitalization or death. Patients who were underweight, with a BMI around 15, were 20 percent more likely to be hospitalized for COVID-19 compared to those with a healthy weight.
... other than age, being overweight may be the most dangerous factor that leads to hospitalization and death from COVID-19
“Continued strategies are needed to ensure community access to nutrition and physical activity opportunities that promote and support a healthy BMI,” the CDC report concludes. “Preventing COVID-19 in adults with higher BMIs and their close contacts remains important and includes multifaceted protection measures such as masking, as well as continued vaccine prioritization and outreach for this population.”
An expansive report from the World Obesity Federation, published in early March, looked at COVID-19 mortality rates across more than 160 countries. The report reveals those countries with more than 50 percent of the population classified as overweight displayed dramatically higher rates of death.
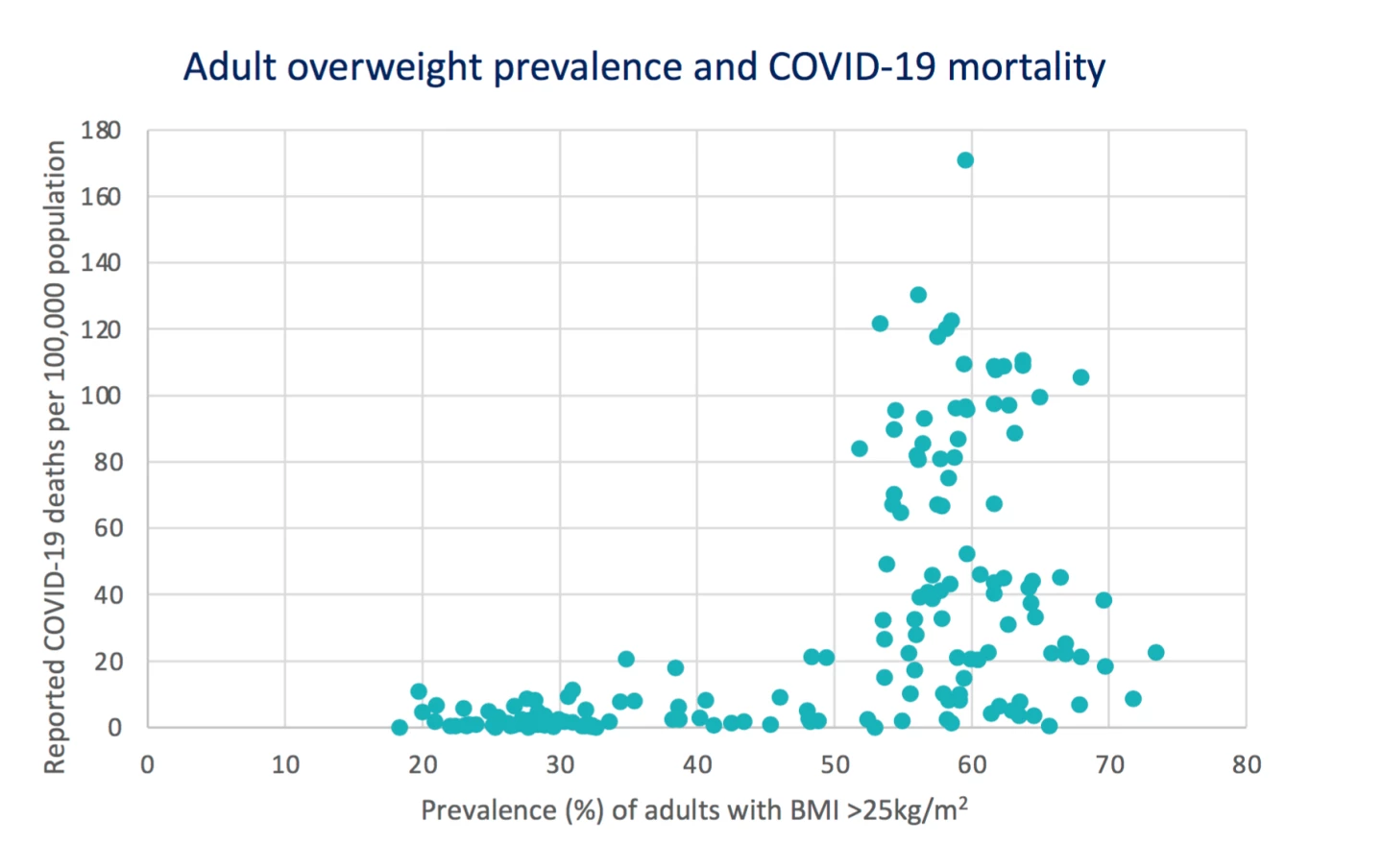
The report describes the non-linear association as remarkable, with mortality rates 10 times higher in countries where over half that population has a BMI higher than 25. It also suggests the association is not due to factors such as better reporting of COVID-19 deaths, national wealth, or overall proportions of older citizens. However, the report is cautious to note the association is a generalization, albeit a deeply striking one.
“We were shocked to see such a high correlation between a country’s proportion of overweight adults and its deaths from COVID-19,” said Tim Lobstein, one of the report’s authors in an interview with The Guardian. “There are rich countries with low levels of overweight, like Japan and South Korea, and they have very low COVID death rates. Equally, there are lower-income countries like South Africa and Brazil, where overweight is now affecting more than half the population, where we see high COVID-19 death rates. We now know that an overweight population is the next pandemic waiting to happen.”
The association between obesity and severe disease is so strong that at least 29 states in the US have included obesity as a qualifying risk factor for the first stage of vaccine roll-out. In those states, citizens with a BMI higher than 30 are eligible to move to the front of the queue for COVID-19 vaccination.
A most important question some researchers are now asking is whether current COVID-19 vaccines will be completely effective in obese individuals. A yet to be peer-reviewed study published as a pre-print in February suggested antibody responses were blunted in overweight and obese subjects following COVID-19 vaccination.
Cate Varney, from the University of Virginia, discussed the issue in a recent piece in The Conversation suggesting prior research has indicated obese subjects may not respond as effectively to some vaccines as those with a healthy weight. It’s unclear what this means in real terms for COVID-19 vaccine efficacy, but she plausibly speculates how a high BMI can disrupt healthy immune functions.
“Although patients with obesity can produce adequate antibodies, multiple studies show they have a lower level of those B and T cells following an infection with the H1N1 influenza,” Varney writes. “This can alter the typical immune response, leaving the body one step behind after the virus invades. An important question is whether this altered immune response is also present after a COVID-19 infection. And because of this, we want to know whether the vaccine will be as effective in patients with obesity for as long as other patients who do not suffer from this disease.”
As researchers around the world gather more and more data, connections between BMI and COVID-19 will become clearer. Nevertheless, a year into this global pandemic and the evidence strongly suggests being overweight or obese puts one at greater risk of severe disease.
The World Obesity Federation report (pdf) can be found here.
The CDC BMI report was published here.





