After a heart attack occurs, non-beating scar tissue forms on the part of the organ that was affected – and this can lead to heart failure. There could be new hope, however, in the form of an implanted device that delivers medication directly to that tissue.
Ordinarily, heart-healing medication is administered either to the body as a whole, or it's injected directly into the heart.
In the case of the former, doses need to be kept fairly low, in order to minimize side effects elsewhere in the body. As a result, relatively small amounts of the medication actually reach the heart. In the case of the latter, multiple injections to the heart are typically required, involving multiple surgeries to access the organ.
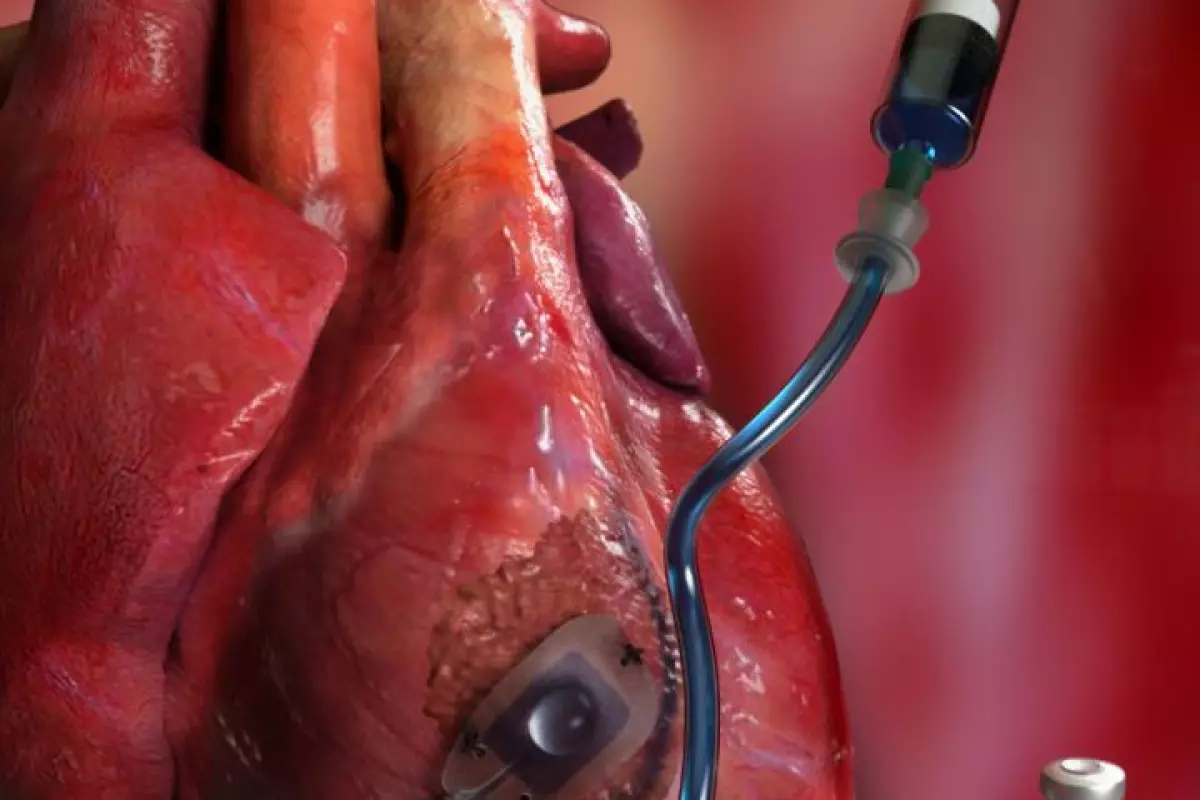
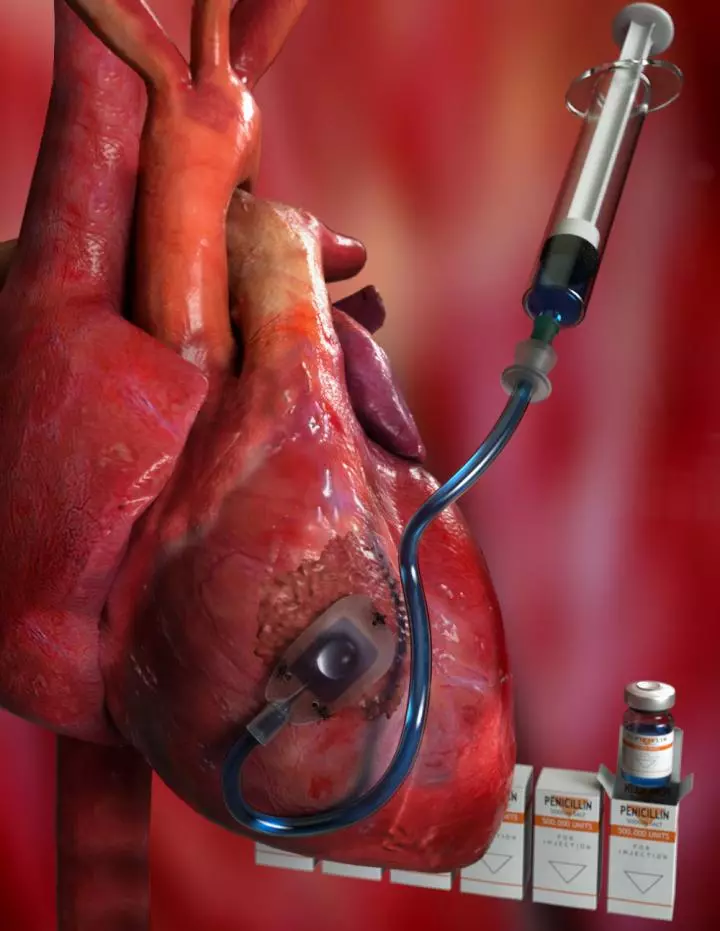
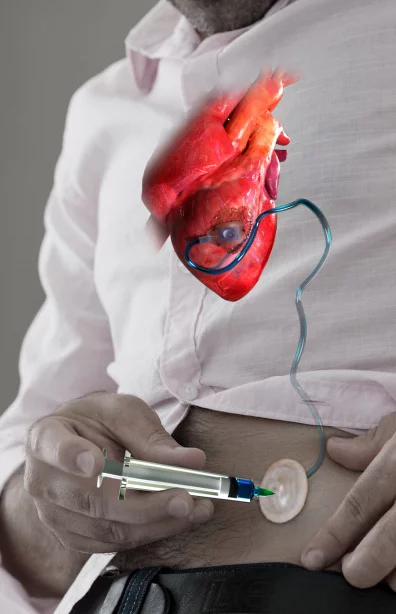
That's where the new Therepi device comes in. Developed by a team of American and Irish scientists, it consists of a thin flexible tube with a small polymer reservoir at the end. That reservoir, which is semi-spherical with a flat underside, gets sutured to the scar tissue on the heart. The tube is routed up to an opening in the patient's skin.
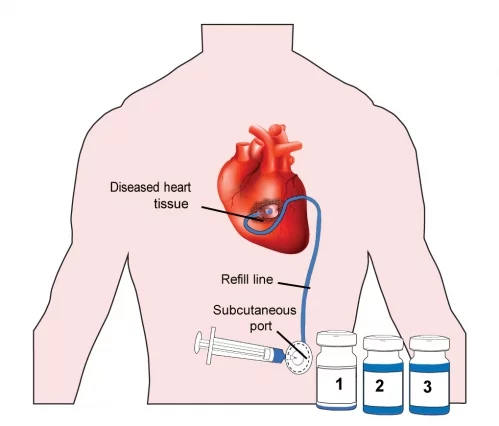
Multiple doses of medication can subsequently be manually pumped in at that skin "port," travelling down the tube and into the reservoir. Because the underside of that reservoir is made of a spongey, permeable polycarbonate membrane, the medication is gradually released through it and straight into the tissue.
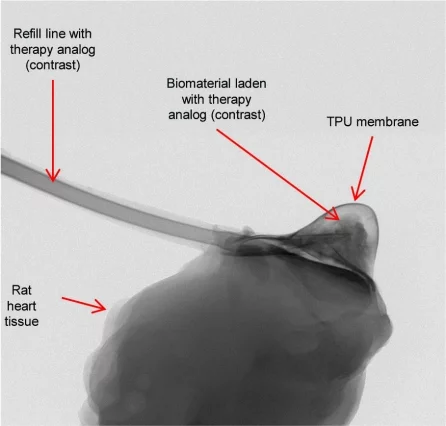
In lab trials, Therepi was successfully used to deliver stem cell-based medication to the scarred hearts of rats, over the course of a month.
"The stem cells remain in the reservoir and act as production factories, constantly releasing factors that are transported out of the device and modulate healing," says MIT assistant professor Ellen Roche. "With multiple replenishments, the 'dose' of these factors is increased, as is their potential to elicit a functional benefit. At 28 days, we observed, among other cardiac parameters, an increased ejection fraction, meaning the percentage of blood ejected compared to total volume of chamber increased."
By contrast, there was little change in hearts that received either a single dose of the stem cells, or that received no treatment at all. It is now hoped that Therepi could ultimately be used not just on human hearts, but also as a means of delivering medication directly to other organs. Additionally, we're told that a biodegradable version is in the works, that wouldn't need to be removed via a second surgery.
The research was led by Harvard University, and along with MIT also involved scientists from the Royal College of Surgeons in Ireland, Trinity College Dublin/AMBER, and the National University of Ireland Galway. A paper on the study was recently published in the journal Nature Biomedical Engineering.
Sources: Harvard University, MIT